Every fall, Medicare Advantage organizations face the same reality: large-scale website updates are tied to Annual Enrollment Periods (AEP).
Benefits finalize late, CMS marketing requirements shift, compliance teams circulate updated disclaimer language, legal review queues back up, and digital teams start duplicating pages to manage county-level variations. And suddenly, hundreds, sometimes thousands, of updates need to go live before AEP opens.
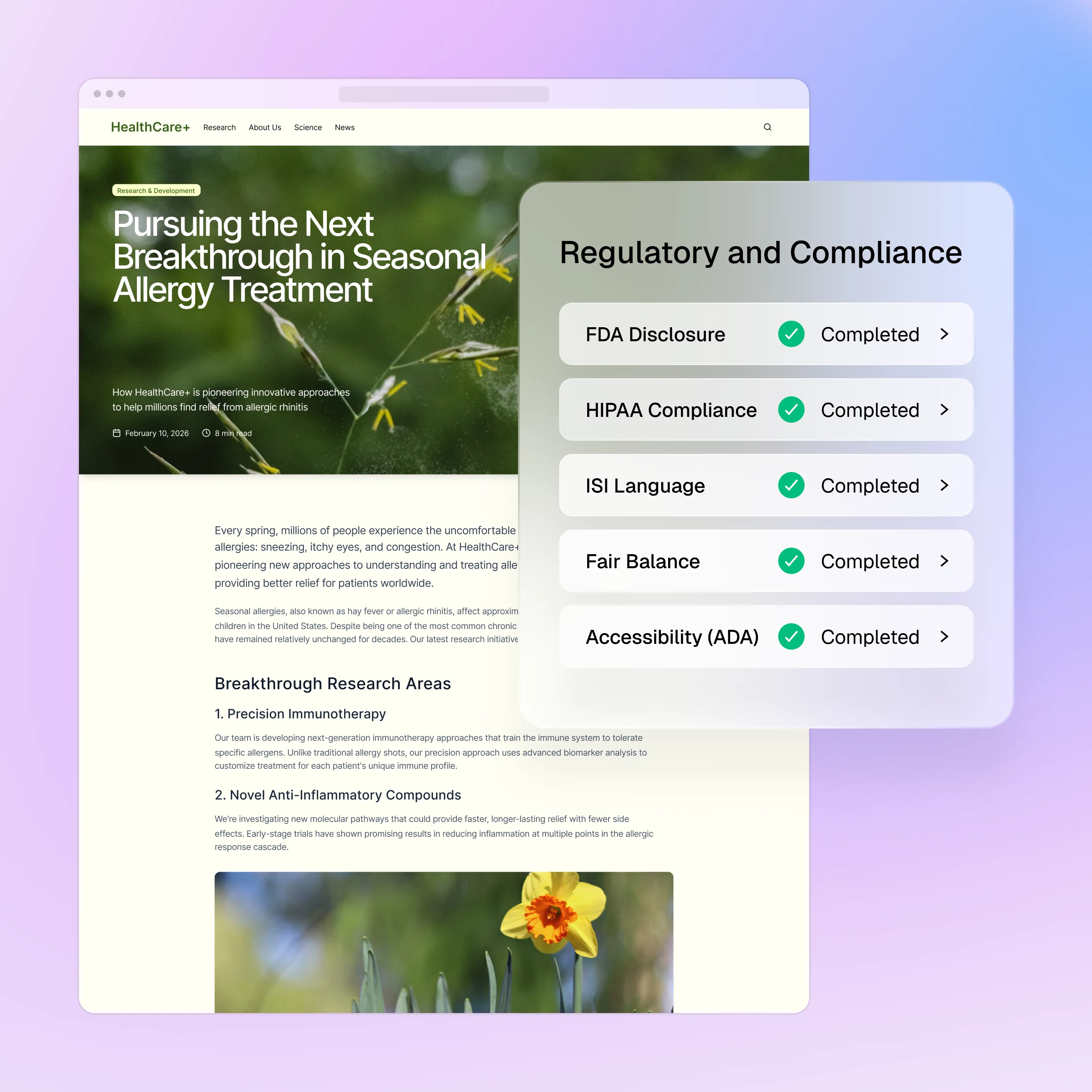
You know what happens next: QA goes manual. Evidence of Coverage and Summary of Benefits PDFs get revised one at a time. Star ratings need refreshing across every plan page. CMS-required disclaimers have to match exact language. Provider directories have to reflect the latest network changes.
Every update carries compliance risk, and every manual touchpoint is a place where something slips. The updates themselves aren’t complex; what’s complex is the waiting: the queues, the handoffs, the serial review chains, the spreadsheet tracking, and the manual sweeps. The work isn’t slow because the work is hard, it’s slow because the work waits.
This cycle repeats every year for Medicare Part C and Part D sponsors. And while many teams treat it as a seasonal surge, the underlying problem isn’t volume, it’s structural.